Depending on where you have your blood taken, a doctor, nurse, or trained phlebotomist will take your blood. In this picture, the phlebotomist has inserted the syringe into a vein on the outer portion of the arm near the elbow.
Follow That Sample: A Short Lab Tour
For you as the patient, the "laboratory test" that has been requested by your doctor may require you to have a sample of blood taken from a vein in your arm, or to give a sample of urine, a swab from your throat or another sample of body fluid or even tissue (a biopsy). Once you have provided the sample, your part of the "lab test" is finished – but the real test happens in the laboratory where trained doctors and scientists analyse the sample on specialised instruments and/or examine the specimens under the microscope. Let's look at a couple of examples: a blood sample and a throat culture.
-
Collecting
-
Labelling
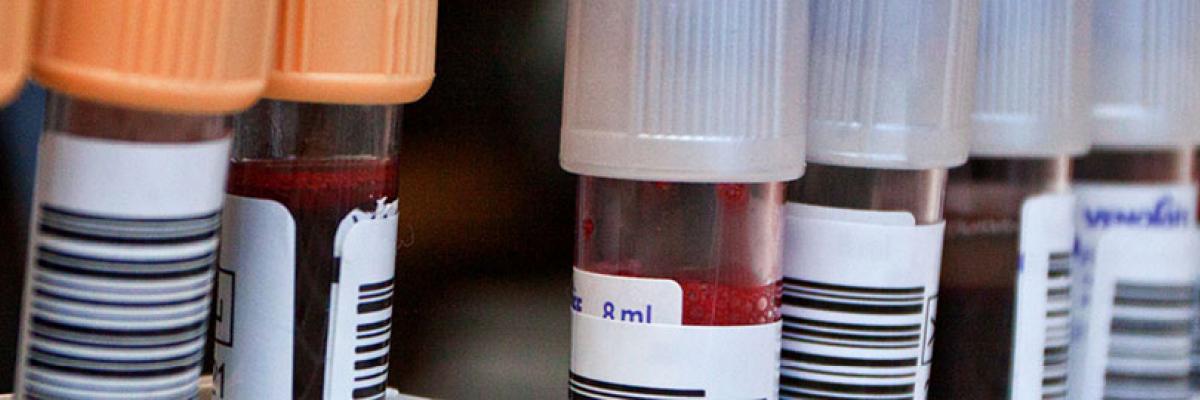
Once the blood is taken, the tube is labelled. Often the label will be pre-printed with the patient's name, and identification number. It is essential that the tube is properly labelled before the phlebotomist leaves the patient’s side and sends the sample to the laboratory. The person taking the blood must always confirm the name of the patient before taking the sample.
-
Documenting
After the sample has been collected and labelled, it is transported to the lab to be booked in. Depending on the test needed and where you have the sample taken, your blood may go to the laboratory in the local hospital, or it may be sent to a laboratory that specialises in analysing samples for a particular test and interpreting the results.
Once the specimen arrives in the lab, however near or far away, your blood sample will be booked into the laboratory's computer system. The tube label contains all the information necessary to ensure that the sample is analysed for all the tests requested and the results are matched to your name.
-
Analysing
In most cases, an automated instrument analyses the blood sample. In this picture, the tube of blood is being placed directly into the machine. This particular state-of-the-art analyser is capable of running batches of samples - up to 120 samples per hour. Some analysers use whole blood as the sample, while others use the serum or plasma that the blood cells float in. For these analysers, the blood sample is centrifuged (span) before testing so the cells sink to the bottom of the tube and the clear serum or plasma can be analysed.
-
Results
With the latest technology in laboratory analysers comes the ability to generate the results electronically and for some tests graphically as well. The results are printed and then sent to the doctor. If the results indicate the patient may be very ill, the laboratory will call the doctor with the results.
The length of time between taking the blood sample and when the doctor gets the results can vary greatly, from as little as an hour to as much as several weeks. Urgency, distances, the complexity of the test, and other factors explain why it may sometimes take so long to get your results.
-
Collecting
-
Labelling
-
Documenting
After the sample has been labelled, it is transported to the lab where it will be booked in. Once it arrives in the laboratory, however near or far away, the sample will be recorded in the laboratory's tracking system. The label contains all the information necessary to ensure that the results of the test on the sample are matched to the correct person.
-
Preparing
-
Incubating
The sealed, labelled petri dish is placed in an incubator, which is a chamber that maintains a constant temperature and other conditions that are optimal for the growth of the bacteria. The culture usually remains in the incubator for 24 - 36 hours to allow sufficient time for any bacteria that may be present to grow
-
Examining
After the incubation, a scientist will visually examine the culture. Some bacteria have a characteristic appearance that enables the laboratory scientist to identify the specific bacteria. In some situations, additional tests may be needed to make the identification. Not all bacteria are harmful and require treatment.
-
Testing for treatment
If harmful bacteria have been identified in the throat culture, the laboratory will do additional tests using different types of antibiotics to see which one is most likely to stop the infection. This test starts by coating the surface of another agar dish with the bacteria. Known concentrations of antibiotics that have been absorbed into white paper discs are placed on the plate. If an antibiotic stops the bacteria on the plate from growing, it appears as a clear halo around the disc. This tells the doctor which antibiotic they can prescribe to cure the throat infection.
-
Getting results




