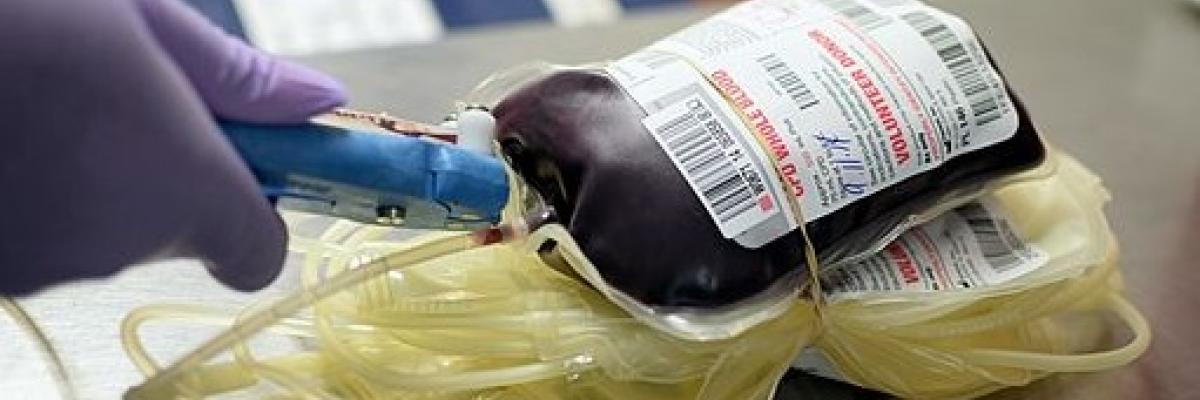
Donating Blood
Who can donate blood?
Blood donors are volunteers who are providing a greatly needed service. About 4 million patients receive blood transfusions each year, and approximately 9,000 units of red blood cells are needed every day. Although 14 million blood units are donated a year, more volunteers are needed to keep the blood supply at an adequate volume.
Donors must meet certain criteria to ensure their safety and the safety of the recipients. These are available on the NBS website
Donors must be:
- 17-59 years of age
- in good health
- weigh at least 50 Kg (7st 12lb), and
- pass a physical and health history examination prior to donation
The physical examination includes measurement of weight, blood pressure, pulse, and temperature as well as a test for anaemia, which requires just a few drops of blood from your finger.
To protect the health of both the donor and the recipient, the health history questionnaire asks about potential exposure to transfusion-transmissible diseases, such as viruses like HIV, hepatitis B and C, as well as parasites that cause diseases such as malaria.
Certain people are not permitted to donate blood for health concerns. This includes:
- Anyone who has ever injected or been injected illegal or body-building drugs
- Men who have had sexual contact with other men
- Patients with haemophilia
- Anyone with a positive test for HIV, or anyone who thinks they might be HIV positive
- Men and women who have engaged in sex for money or drugs
- Anyone who has had hepatitis B or C virus
- Anyone who has had a previous blood transfusion
- Anyone who has had acupuncture, body piercing or a tattoo in the last 12 months
- Anyone who has two family members with Crueutzfeldt-Jakob disease (CJD)
There also may be some restrictions if you are taking certain medications at the time of donation. You may be ineligible to donate or deferred for a period of time. There are also varying deferral periods if you have been vaccinated recently. For a more details visit the NBS website.
Donors have a personal responsibility to help ensure the safety of the blood supply. You should express any concerns or questions you may have about past illnesses you had or may have been exposed to before donating. Who knows, it is possible that maybe someone close to you will be the recipient of your blood donation.
Where can blood be donated?
Blood can be donated at blood transfusion centres, or mobile sites temporarily set up in public areas like colleges, workplaces, and churches. There are hundreds of institutions involved in blood banking throughout the UK.
For more information on where you can go to donate or receive blood, visit the NHSBT website.
What is donated and how often?
Usually one unit of 475mL (just under a pint) of blood is collected into a blood bag from a vein in the inner part of the elbow joint using a new, sterile needle. Your body replenishes the fluid lost during donation in 24 hours, but it may take up to 2 months to replace the lost red blood cells. Therefore blood can usually be donated only once every 16 weeks.
What are the components of blood?
Blood is made up of several components. These components can be separated in the laboratory so that they can be transfused into multiple patients, each with different needs, since rarely will a person need all of the components within whole blood. These components include:
- Red blood cells – main cellular element in the blood; carry oxygen to the body tissues; used in the treatment of anaemia resulting from, for example, kidney failure, gastrointestinal bleeding, or blood loss during trauma or surgery
- Platelets – cellular elements needed for blood to clot; used in the treatment of leukaemia and other types of cancer and conditions in which patients have a shortage of platelets (e.g., thrombocytopenia) or abnormal platelet function to control bleeding
- Plasma – straw-coloured fluid part of blood in which the red and white blood cells and platelets are suspended; helps to maintain blood pressure and the fluid-electrolyte and acid-base balances of the body and transport wastes; used to help control bleeding when no coagulation factor-specific concentrate is available
- Cryoprecipitate – is prepared from plasma and contains fibrinogen
- White blood cells – cellular elements that fight infection and function in the immune process, one type, called granulocytes, can be transfused to fight infections that are unresponsive to antibiotic therapy, although the effectiveness of this form of treatment is still being investigated
Separation of these components is performed by first treating the blood to prevent clotting and then letting the blood stand. Red blood cells settle to the bottom, while plasma migrates to the top. Using a centrifuge to spin out these components can speed up the process. The plasma is then removed and placed in a sterile bag. It can be used to prepare platelets, plasma, and cryoprecipitate, again with the help of a centrifuge to separate out the platelets. Plasma may be pooled with that from other donors and processed further (fractionated) to provide purified plasma proteins, such as albumin, immunoglobulin, and clotting factor concentrates.